The grade and stage of prostate cancer can help stratify risk
Conduct risk stratification to optimize patient care
- Assessing prostate-specific antigen (PSA) levels
- Grade of the tumor
- Extent of the cancer revealed by biopsy
- Stage of cancer
- Spread of cancer
PSA tests can reveal recurrence and give an indication of the cancer’s growth.

Consider the value of the PSA along with the patient’s age and size of prostate, as a larger prostate could yield a higher PSA value. Calculate the PSA density (PSAD) by dividing PSA level by prostate volume. A value of ≥0.15 may require further evaluation.
Tumor grade
1
Small, identical cells that are close together
2
Cells in various shapes and sizes, loosely packed
3
Increased cell size with irregular shapes; cells
are closer together
4
Large, irregular, fused cells
5
Irregular, fused cells that have invaded
surrounding connective tissue cells
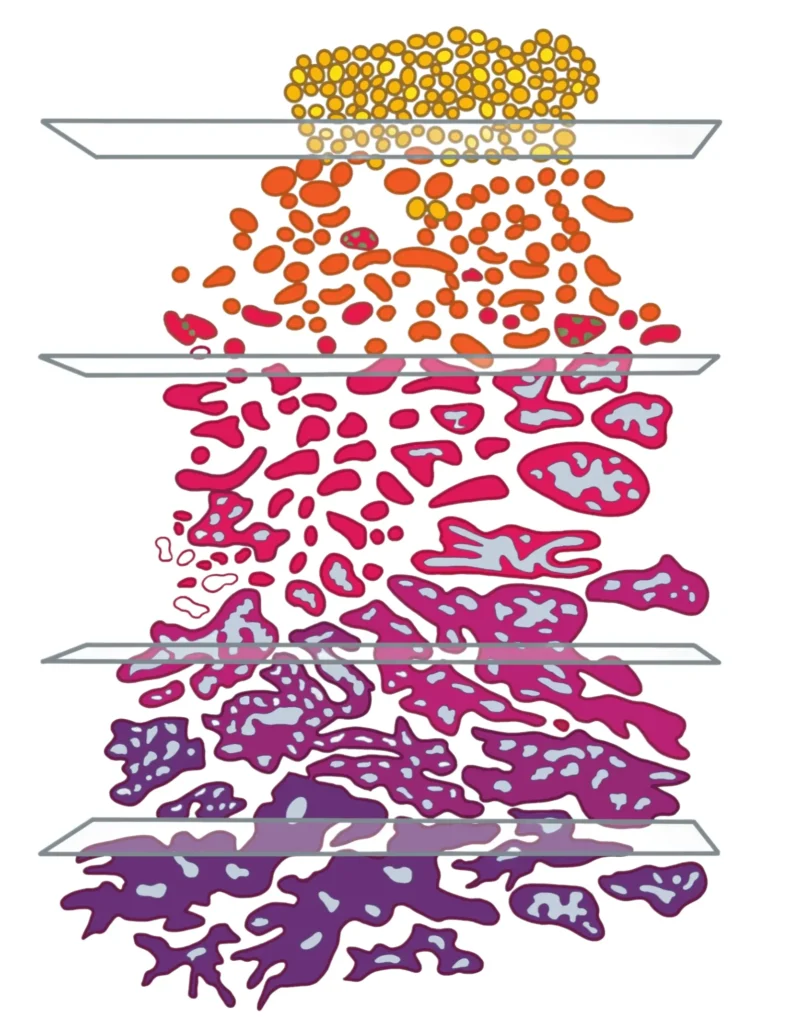
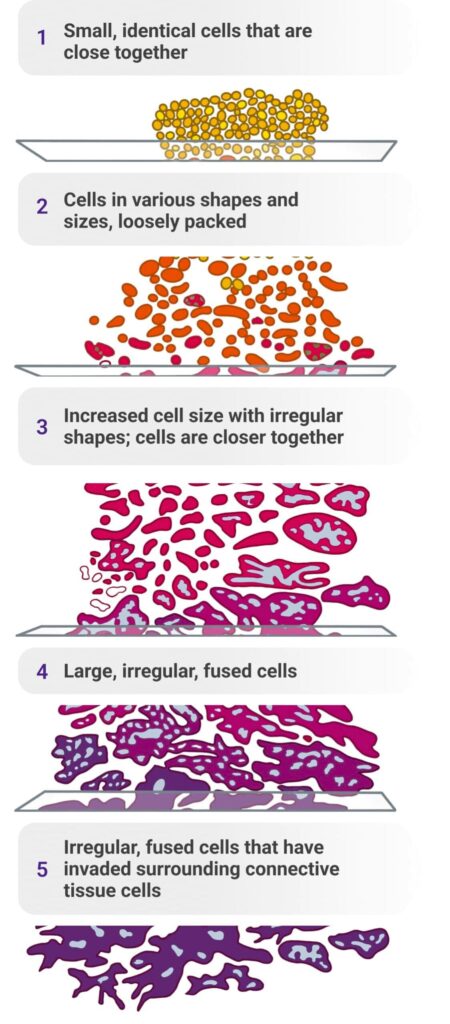
Gleason score is determined by grading the two most common cell types (Gleason patterns) found during biopsy. These are then added together for a score. Scores range from 6-10, with 6 being more normal and low risk and 10 being very abnormal and higher risk.5
See how to stratify risk for prostate cancer based on certain criteria by reviewing the accompanying table.
| Prostate cancer risk stratification7* | |
|---|---|
| Risk Profile | Criteria† |
| Favorable: very low risk | T1c, Gleason score ≤6, PSA level <10 ng/mL, PSA density <0.15 ng/mL/mL, <3 biopsy cores positive, ≤50% cancer in any core |
| Low risk | T1 or T2a, Gleason score 2-6, PSA level <10 ng/mL |
| Intermediate | T2b - T2c or Gleason score 7 or PSA level 10-20 ng/mL |
| High | T3a or Gleason score 8-10 or PSA level >20 ng/mL |
*Adapted from: D’Amico et al. and Epstein et al.
†Adapted from: Mohler J et al. and based on T-stage, Gleason score, PSA level, PSA density, number and percentage of biopsy cores with cancer.
